Breast tissue changes throughout the month in adult women. Some changes are normal, but some may require a provider’s attention. It is important that you know the signs and symptoms of breast cancer. When it is discovered early, you have more treatment options and a better chance for long-term survival. In fact, when breast cancer is diagnosed and treated in its early stages, the five-year survival rate is 95 percent. Most breast lumps are not cancerous. Yet the most common sign of breast cancer for both men and women is a lump or thickening in the breast. Often, the lump is painless.
Breast Care Services
At Waverly Health Center, breast care is about more than imaging and procedures. It’s about listening, compassion and confidence in your care. From routine screenings to advanced diagnostic services, our experienced team is here to support you.
We understand that breast health appointments can bring uncertainty. That’s why we focus on creating a calm, supportive environment where your questions are welcomed and your comfort matters.
Contact Us
Phone: (319) 483-4074
Fax: (800) 447-5890
Director: Nicole Myers, Chief Clinic Officer
Medical Director: Dr. Ann Rathe
Hours & Additional Information
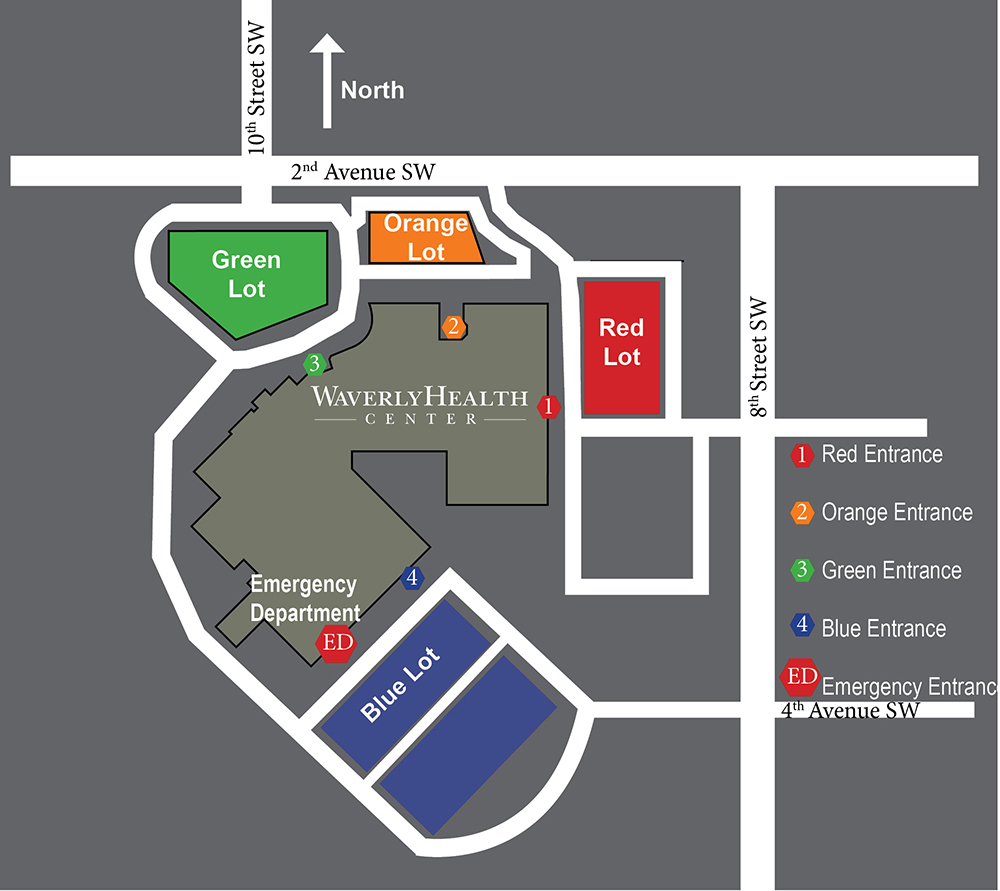
Please park in the green parking lot and enter through the green entrance.
Breast Cancer Risk Factors
What to Expect
We want you to feel informed, comfortable and supported throughout your visit. Here’s what you can expect when you come to Waverly Health Center for breast care services.
Before Your Appointment: Our team will help you prepare for your visit. You may receive instructions about what to bring with you.
When You Arrive: You’ll be welcomed by a caring team who understands that breast care appointments can feel personal. We strive to create a calm, respectful environment.
During Your Exam: Your exam will be explained step-by-step so you know what’s happening and why. Our trained team will prioritize your comfort and privacy and will work with you to make the experience as smooth as possible.
After Your Appointment: If additional testing or follow-up is recommended, our team will guide you through next steps and help coordinate care.
Our Providers
Frequently Asked Questions
What should every woman know about their breasts and their individual risk?